Metabolome alterations in pediatric metabolically unhealthy obesity are primarily linked to abnormal glucose homeostasis
Clinical metabolic parameters of children and adolescents without obesity, children and adolescents with MHO, and children and adolescents with MUO
Children and adolescents with obesity had significantly higher adiposity measures (BMI z-score and body fat percentage), fasting insulin, fasting glucose, homeostatic model assessment for insulin resistance (HOMA-IR), systolic blood pressure (SBP), triglycerides (TG) and significantly lower HDL cholesterol than children and adolescents without obesity (Supplementary Table 1).
Apart from significant differences in adiposity measures, children and adolescents with MHO exhibited significantly higher fasting insulin (19.6 mU/L (11.9–26.0) vs 5.80 mU/L (5.20–9.70)) and HOMA-IR (4.08 (2.58–5.59) vs 1.19 (1.00–2.02)) compared to children and adolescents without obesity. Conversely, children and adolescents with MUO had significantly higher fasting insulin (25.7 mU/L (17.4–36.0) vs 5.80 mU/L (5.20–9.70)), HOMA-IR (5.65 (3.58–7.67) vs 1.19 (1.00–2.02)), SBP (124 mmHg (116–131) vs 111 mmHg (103–119)), TG (1.29 mmol/L (0.99–1.90) vs 0.85 mmol/L (0.57–1.22)) and lower HDL cholesterol (1.05 mmol/L (0.95–1.19) vs 1.39 mmol/L (1.16–1.61)) than children and adolescents without obesity (Table 1).
Children and adolescents with MHO were significantly younger (13.1 years (10.1–15.4) vs 15.1 years (13.2–16.5)) and exhibited significantly lower fasting insulin (19.6 mU/L (11.9–26.0) vs 25.7 mU/L (17.4–36.0)), 2-h oral glucose tolerance test (OGTT) (5.80 mmol/L (5.30–6.40) vs 6.30 mmol/L (5.30–7.40)), C-peptide (797 pmol/L (672–800) vs 1047 pmol/L (800–1279)), HOMA-IR (4.08 (2.58–5.59) vs 5.65 (3.58–7.67)), SBP (111 mmHg (104–118) vs 124 mmHg (116–131)), diastolic blood pressure (DBP) (61 mmHg (57–67) vs 67 mmHg (61–71)), TG (1.01 mmol/L (0.79–1.27) vs 1.29 mmol/L (0.99–1.90)), and higher HDL cholesterol (1.22 mmol/L (1.15–1.34) vs 1.05 mmol/L (0.95–1.19)) than their MUO counterparts (Table 1).
Proportion of children and adolescents with MUO for each metabolic syndrome criteria
Among the children and adolescents with MUO, 47.8% were found to have two or more MetS criteria (Supplementary Fig. 1A). According to each MetS criteria, 48.6% had elevated blood pressure, 32.0% had hypertriglyceridemia, 55.9% had dyslipidaemia (abnormal HDL) and 26.1% had abnormal glucose tolerance (AGT) (Supplementary Fig. 1B).
Plasma metabolome of children and adolescents without obesity, children and adolescents with MHO and children and adolescents with MUO
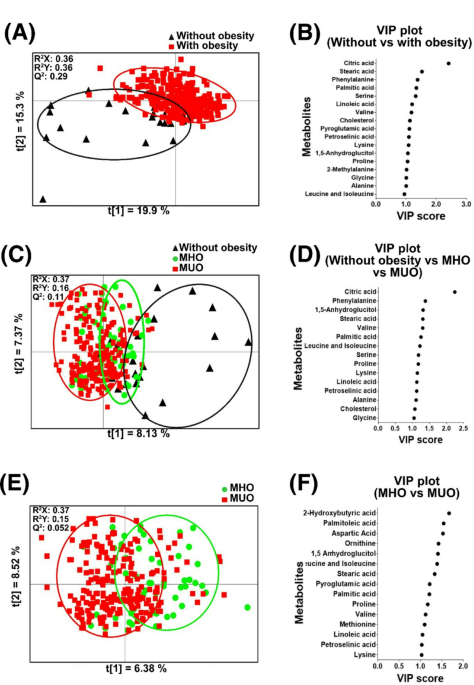
Untargeted gas chromatography-time of flight mass spectrometry (GC-TOF/MS) metabolomic profiling of plasma metabolites in children and adolescents without obesity, those with MHO and those with MUO detected 60 putative metabolites, primarily consisting of FA, AA and their downstream metabolites, as detailed in Supplementary Table 2. Supervised partial least square discriminant analysis (PLS-DA) of plasma metabolome showed a discrimination between children and adolescent without obesity and those with obesity (R2X: 0.36, R2Y: 0.36, Q2: 0.29) (Fig. 1A). The corresponding variable importance in projection (VIP) plot revealed a metabolite signature rich in AA (BCAA, phenylalanine, lysine, serine, 2-methylalanine, proline, glycine and alanine), saturated FA (palmitic and stearic acid), unsaturated FA (linoleic and petroselinic acid), citric acid, cholesterol and 1,5-anhydroglucitol (Fig. 1B). Pairwise analysis revealed that children and adolescents without obesity had significantly higher concentrations of 1,5-anhydroglucitol, citric acid, leucine, isoleucine, stearic acid, glycine, serine, pyroglutamic acid and cholesterol and lower concentrations of 2-methylalanine than those with obesity (Supplementary Table 3).
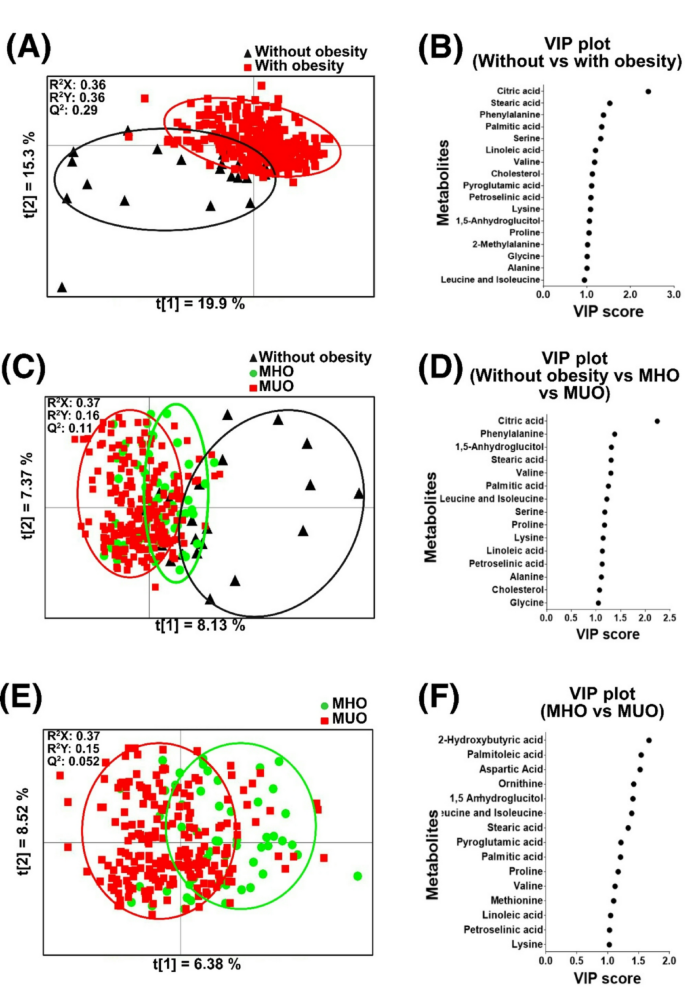
Multivariate data analysis of plasma metabolites distinguishing between children and adolescents without obesity, those with MHO, and those with MUO. The PLS-DA plot depicts plasma metabolites that discriminate between (A) children and adolescents without obesity and those with obesity, (C) children and adolescents without obesity, those with MHO, and those with MUO, and (E) children and adolescents with MHO versus those with MUO. The Variable Importance in Projection (VIP) plots highlight important metabolites (VIP score > 1) that distinguish between (B) children and adolescents without obesity and those with obesity, (D) children and adolescents without obesity, those with MHO, and those with MUO, and (F) children and adolescents with MHO versus those with MUO. MHO: metabolically healthy obesity, MUO: metabolically unhealthy obesity. MHO: metabolically healthy obesity, MUO: metabolically unhealthy obesity.
Plasma metabolome also distinguished between children and adolescents without obesity, those with MHO and those with MUO (R2X: 0.37, R2Y: 0.16, Q2: 0.11) (Fig. 1C). The corresponding VIP plot revealed metabolites similar to those identified in the distinction between children and adolescents without obesity and those with obesity (Fig. 1D). Children and adolescents without obesity had significantly higher concentrations of citric acid, serine and lower concentrations of phenylalanine compared to those with MHO (Supplementary Table 4). In contrast, children and adolescents without obesity were found to have significantly higher concentrations of 1,5-anhydroglucitol, citric acid, stearic acid, glycine, serine and cholesterol and lower concentrations of leucine and isoleucine compared to those with MUO (Supplementary Table 4).
Plasma metabolites associated with MUO phenotype
Plasma metabolome was found to discriminate between metabolic health between children and adolescents with MHO and those with MUO (R2X: 0.37, R2Y: 0.15, Q2: 0.052) (Fig. 1E). The discriminatory metabolites with VIP score > 1 consisted of AA (BCAA, aspartic acid, ornithine, pyroglutamic acid, proline, methionine and lysine), saturated FA (palmitic and stearic acid), unsaturated FA (palmitoleic, linoleic and petroselinic acid), 1,5-anhydroglucitol and 2-hydroxybutyric acid (Fig. 1F). Children and adolescents with MHO had significantly higher concentrations of 1,5-anhydroglucitol, petroselinic acid, palmitoleic acid, 2-hydroxybutyric acid, aspartic acid and ornithine than those with MUO (Supplementary Table 5).
Correspondingly, lower concentrations of 1,5-anhydroglucitol, palmitoleic acid, petroselinic acid, 2-hydroxybutyric acid, aspartic acid and ornithine were found to be significantly associated with the MUO phenotype after adjusting for race, sex, age and BMI z-score (Supplementary Fig. 2).
Plasma metabolites associated with MetS criteria and cardiometabolic parameters among children and adolescents with MUO
We found that only higher concentrations of pyroglutamic acid (OR: 1.22, 95% CI: 1.00–1.49; p = 0.048) was marginally associated with dyslipidaemia (abnormal HDL). Lower concentrations of 1,5-anhydroglucitol (OR: 0.19, 95% CI: 0.06–0.54; p = 0.002) and higher concentrations of BCAA, including valine (OR: 1.34, 95% CI: 1.05–1.72; p = 0.02), leucine and isoleucine (OR: 1.41, 95% CI: 1.10–1.80; p = 0.006), 2-hydroxybutyric acid (OR: 3.74, 95% CI: 1.24–11.3; p = 0.02) and lysine (OR: 4.10, 95% CI: 1.31–12.9; p = 0.016) were significantly associated with AGT (Table 2). There were no metabolites significantly associated with elevated blood pressure and hypertriglyceridemia.
Aspartic acid (r = 0.171, p = 0.014) and ornithine (r = 0.143, p = 0.041) were significantly positively correlated with SBP (Table 3). 2-Hydroxybutyric acid (r = 0.156, p = 0.026), leucine and isoleucine (r = 0.197, p = 0.005), valine (r = 0.148, p = 0.035), proline (r = 0.142, p = 0.043), methionine (r = 0.178, p = 0.011), and ornithine (r = 0.198, p = 0.004) were significantly positively correlated with fasting glucose while 1,5-anhydroglucitol (r = − 0.199, p = 0.004) was significantly inversely correlated with 2-h OGTT (Table 3). 1,5-anhydroglucitol (r = − 0.147, p = 0.035), petroselinic acid (r = − 0.224, p = 0.001) and palmitoleic acid (r = − 0.213, p = 0.002) were significantly inversely correlated with HOMA-IR while leucine and isoleucine (r = 0.200, p = 0.004), valine (r = 0.201, p = 0.004), proline (r = 0.170, p = 0.015), methionine (r = 0.205, p = 0.003), lysine (r = 0.236, p = 0.001) and ornithine (r = 0.388, p < 0.001) were significantly positively correlated with HOMA-IR (Table 3).
After stratifying the children and adolescents with MUO by sex, we observed a consistent overall pattern across both sexes, with metabolomic perturbations primarily associated with abnormal glucose homeostasis (Supplementary Tables 6 to 9). However, notable sex-specific differences emerged in individual metabolite associations. In males with MUO, lower plasma 1,5-anhydroglucitol was significantly associated with AGT (Supplementary Table 6), and discriminatory metabolites were more strongly linked to fasting glucose (Supplementary Table 7). In contrast, in females with MUO, higher plasma BCAA, methionine, and lysine were significantly associated with AGT (Supplementary Table 8), and discriminatory metabolites were primarily associated with HOMA-IR (Supplementary Table 9).
Plasma metabolome of children and adolescents with obesity and normal glucose tolerance (NGT) and children and adolescents with obesity and AGT
Plasma metabolome of children and adolescents with obesity and NGT could be differentiated from those with obesity and AGT (R2X: 0.38, R2Y: 0.22, Q2: 0.054) (Fig. 2A). The corresponding VIP plot identified 1,5-anhydroglucitol, glyceric acid, palmitoleic acid, leucine, isoleucine, valine, 3-hydroxyisobutyric acid (3-HIB), 2-methylalanine, lysine, methionine, and aspartic acid as key metabolites differentiating between these groups (Fig. 2B).

Multivariate data analysis of plasma metabolites that discriminate between children and adolescents with obesity and NGT and those with obesity and AGT. (A) PLS-DA plot illustrates the plasma metabolites that discriminate between children and adolescents with obesity and NGT and those with obesity and AGT. (B) Variable Importance in Projection (VIP) plot highlights key metabolites with VIP scores greater than 1 that distinguish between children and adolescents with obesity and normal glucose tolerance (NGT) and those with obesity and abnormal glucose tolerance (AGT). AGT: abnormal glucose tolerance, NGT: normal glucose tolerance.
Children and adolescents with obesity and AGT had significantly higher concentrations of leucine and isoleucine (p = 0.01) and 3-HIB (p = 0.003) and significantly lower concentrations of 1,5-anhydroglucitol (p < 0.001), glyceric acid (p = 0.015) and aspartic acid (p = 0.027) than those with obesity and NGT (Fig. 3 and Supplementary Table 10).

Fold change (FC) of important plasma metabolite levels (VIP score > 1) in the AGT group relative to the NGT group (with FC set to 1 for NGT). Middle, lower and upper limits of the box plot represent median and IQR (25th and 75th percentile) respectively. Red boxes denote significantly elevated metabolites, while blue boxes indicate significantly reduced metabolites in the AGT group compared to the NGT group. *: p < 0.05; **: p ≤ 0.01; ***: p < 0.001. 1,5-AHG: 1,5-Anhydroglucitol; 3-HIB: 3-Hydroxyisobutyric acid; AA: Amino acid; BCAA: Branched-chain amino acids; FA: Fatty acids.
link