Characterizing everyday exposure to volatile organic compounds and upper respiratory health effects
World Health Organization. WHO Global Air Quality Guidelines. Particulate Matter (PM2.5 and PM10), Ozone, Nitrogen Dioxide, Sulfur Dioxide and Carbon Monoxide. (2021).
Sierra-Vargas, M. P. & Teran, L. M. Air pollution: impact and prevention. Respirol. Carlton Vic. 17, 1031–1038 (2012).
Google Scholar
Liu, C. et al. Ambient Particulate Air Pollution and Daily Mortality in 652 cities. N Engl. J. Med. 381, 705–715 (2019).
Google Scholar
Costantini, A. S. et al. Risk of leukemia and multiple myeloma associated with exposure to benzene and other organic solvents: evidence from the Italian Multicenter Case-control study. Am. J. Ind. Med. 51, 803–811 (2008).
Google Scholar
Madani, N. A., Jones, L. E. & Carpenter, D. O. Different volatile organic compounds in local point source air pollution pose distinctive elevated risks for respiratory disease-associated emergency room visits. Chemosphere 344, 140403 (2023).
Google Scholar
Hester, S. D., Johnstone, A. F. M., Boyes, W. K., Bushnell, P. J. & Shafer, T. J. Acute toluene exposure alters expression of genes in the central nervous system associated with synaptic structure and function. Neurotoxicol Teratol. 33, 521–529 (2011).
Google Scholar
Chen, D. et al. Exposure to benzene, occupational stress, and reduced birth weight. Occup. Environ. Med. 57, 661–667 (2000).
Google Scholar
Liu, N. et al. Health effects of exposure to indoor volatile organic compounds from 1980 to 2017: a systematic review and meta-analysis. Indoor Air. 32, e13038 (2022).
Google Scholar
McGraw, K. E. et al. Exposure to volatile organic compounds – acrolein, 1,3-butadiene, and crotonaldehyde – is associated with vascular dysfunction. Environ. Res. 196, 110903 (2021).
Google Scholar
Liu, W. et al. Single-chemical and mixture effects of multiple volatile organic compounds exposure on liver injury and risk of non-alcoholic fatty liver disease in a representative general adult population. Chemosphere 339, 139753 (2023).
Google Scholar
Lv, J. J. et al. Assessing volatile organic compounds exposure and chronic obstructive pulmonary diseases in US adults. Front. Public. Health. 11, 1210136 (2023).
Google Scholar
Laumbach, R. J. et al. Nasal effects of a mixture of volatile organic compounds and their ozone oxidation products. J. Occup. Environ. Med. 47, 1182–1189 (2005).
Google Scholar
Araki, A. et al. Relationship between selected indoor volatile organic compounds, so-called microbial VOC, and the prevalence of mucous membrane symptoms in single family homes. Sci. Total Environ. 408, 2208–2215 (2010).
Google Scholar
Vineis, P. et al. What is new in the exposome? Environ. Int 143, 105887 (2020).
Hart, J. E. et al. Long-term ambient multipollutant exposures and mortality. Am. J. Respir Crit. Care Med. 183, 73–78 (2011).
Google Scholar
Vermeulen, R., Schymanski, E. L., Barabási, A. L. & Miller, G. W. The exposome and health: where chemistry meets biology. Science 367, 392–396 (2020).
Google Scholar
Sarigiannis, D. A. Assessing the impact of hazardous waste on children’s health: the exposome paradigm. Environ. Res. 158, 531–541 (2017).
Google Scholar
Rappaport, S. M. Redefining environmental exposure for disease etiology. Npj Syst. Biol. Appl. 4, 1–6 (2018).
Google Scholar
Rappaport, S. M. & Smith, M. T. Environ. Disease Risks Sci. 330, 460–461 (2010).
Google Scholar
Vineis, P. & Barouki, R. The exposome as the science of social-to-biological transitions. Environ. Int. 165, 107312 (2022).
Google Scholar
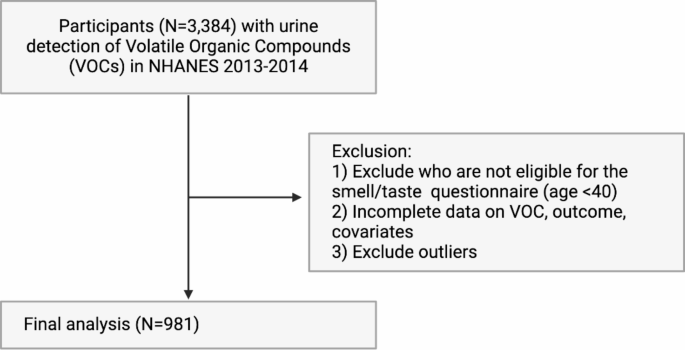
Centers for Disease Control and Prevention (CDC) & National Center for Health Statistics (NCHS). National Health and Nutrition Examination Survey Data (U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2013).
Victor De Jesus & & James, L. Pirkle. Laboratory Procedure Manual: Volatile Organic Compounds (VOCs) Metabolites (Centers for Disease Control and Prevention, 2018).
John Eckfeldt. Laboratory Procedure Manual: Creatinine (University of Minnesota, 2015).
Connie, S. & James, L. Pirkle. Laboratory Procedure Manual: Cotinine and Hydroxycotinine (Total)vol. 2017 (Centers for Disease Control and Prevention, 2016).
Pirkle, J. L. et al. Exposure of the US population to environmental tobacco smoke: the Third National Health and Nutrition Examination Survey, 1988 to 1991. JAMA 275, 1233–1240 (1996).
Google Scholar
Stevens, J. P. Applied Multivariate Statistics for the Social Sciences, Fifth Edition (Routledge, 2012).
Kaiser, H. F. The Application of Electronic Computers to Factor Analysis. Educ. Psychol. Meas. 20, 141–151 (1960).
Google Scholar
Cattell, R. B. The Scree Test for the number of factors. Multivar. Behav. Res. 1, 245–276 (1966).
Google Scholar
Melville, J., Lun, A., Djekidel, M. N., Hao, Y. & Eddelbuettel, D. The Uniform Manifold Approximation and Projection (UMAP) Method for Dimensionality Reduction. (2023).
stuchly stuchly/Rphenoannoy. (2023).
Delgado-Saborit, J. M., Aquilina, N. J., Meddings, C., Baker, S. & Harrison, R. M. Relationship of personal exposure to volatile organic compounds to home, work and fixed site outdoor concentrations. Sci. Total Environ. 409, 478–488 (2011).
Google Scholar
Wang, Y. et al. Associations between the compositional patterns of blood volatile organic compounds and chronic respiratory diseases and ages at onset in NHANES 2003–2012. Chemosphere 327, 138425 (2023).
Google Scholar
Mendy, A. et al. Urinary volatile organic compound metabolites and reduced lung function in U.S. adults. Respir Med. 205, 107053 (2022).
Google Scholar
Norbäck, D., Hashim, J. H., Hashim, Z. & Ali, F. Volatile organic compounds (VOC), formaldehyde and nitrogen dioxide (NO2) in schools in Johor Bahru, Malaysia: associations with rhinitis, ocular, throat and dermal symptoms, headache and fatigue. Sci. Total Environ. 592, 153–160 (2017).
Google Scholar
Pappas, G. P. et al. The respiratory effects of volatile organic compounds. Int. J. Occup. Environ. Health. 6, 1–8 (2000).
Google Scholar
Saijo, Y. et al. Symptoms in relation to chemicals and dampness in newly built dwellings. Int. Arch. Occup. Environ. Health. 77, 461–470 (2004).
Google Scholar
Wieslander, G., Norbäck, D., Nordström, K., Wålinder, R. & Venge, P. Nasal and ocular symptoms, tear film stability and biomarkers in nasal lavage, in relation to building-dampness and building design in hospitals. Int. Arch. Occup. Environ. Health. 72, 451–461 (1999).
Google Scholar
Wolkoff, P., Clausen, P. A., Larsen, S. T., Hammer, M. & Nielsen, G. D. Airway effects of repeated exposures to ozone-initiated limonene oxidation products as model of indoor air mixtures. Toxicol. Lett. 209, 166–172 (2012).
Google Scholar
Venn, A. J. Effects of volatile organic compounds, damp, and other environmental exposures in the home on wheezing illness in children. Thorax 58, 955–960 (2003).
Google Scholar
Stamatelopoulou, A., Asimakopoulos, D. N. & Maggos, T. Effects of PM, TVOCs and comfort parameters on indoor air quality of residences with young children. Build. Environ. 150, 233–244 (2019).
Google Scholar
Kharel, M. et al. Assessing volatile organic compound level in selected workplaces of Kathmandu Valley. Heliyon 7, e08262 (2021).
Google Scholar
Bolden, A. L., Kwiatkowski, C. F. & Colborn, T. New look at BTEX: are ambient levels a Problem? Environ. Sci. Technol. 49, 5261–5276 (2015).
Google Scholar
Athersuch, T. J. & Keun, H. C. Metabolic profiling in human exposome studies. Mutagenesis 30, 755–762 (2015).
Google Scholar
Bouatra, S. et al. The human urine metabolome. PloS One. 8, e73076 (2013).
Google Scholar
Rappaport, S. M., Barupal, D. K., Wishart, D., Vineis, P. & Scalbert, A. The blood exposome and its role in discovering causes of disease. Environ. Health Perspect. 122, 769–774 (2014).
Google Scholar
Agency for Toxic Substances and Disease Registry (ATSDR). Toxic Substances Portal | ATSDR. https://wwwn.cdc.gov/TSP/index.aspx
U.S. Department of Health and Human Services. Public Health Service. Toxicological Profile for Acrylamide. Agency Toxic. Subst. Dis. Regist (2012).
U.S. EPA & SUMMARY REVIEW OF THE HEALTH EFFECTS ASSOCIATED WITH PROPYLENE OXIDE: HEALTH ISSUE ASSESSMENT. US Environ. Prot. Agency EPA (2004). /600/8–86/007F.
Rianto, B. U. D., Yudhanto, D. & Herdini, C. The correlation between length of work and Nasal Mucociliary Transport Time of Gas/Fuel Station Workers. Kobe J. Med. Sci. 64, E6–E10 (2018).
Google Scholar
Biagioni, B., Annesi-Maesano, I., D’Amato, G. & Cecchi, L. The rising of allergic respiratory diseases in a changing world: from climate change to migration. Expert Rev. Respir Med. 14, 973–986 (2020).
Google Scholar
Papadopoulos, N. G. et al. Addressing Adverse Synergies between Chemical and Biological Pollutants at schools—The ‘SynAir-G’ Hypothesis. Allergy n/a.
Yang, J. et al. Association between serum cotinine and volatile organic compounds (VOCs) in adults living with HIV, HBV, or HCV (NHANES 2005–2018). Sci. Rep. 12, 21769 (2022).
Google Scholar
Norbäck, D., Hashim, Z., Ali, F. & Hashim, J. H. Asthma symptoms and respiratory infections in Malaysian students-associations with ethnicity and chemical exposure at home and school. Environ. Res. 197, 111061 (2021).
Google Scholar
Obeng, G. M., Aram, S. A., Agyei, D. & Saalidong, B. M. Exposure to particulate matter (PM2.5) and volatile organic compounds (VOCs), and self-reported health symptoms among fish smokers: a case study in the Western Region of Ghana. PloS One. 18, e0283438 (2023).
Google Scholar
Sheppard, N., Carroll, M., Gao, C. & Lane, T. Particulate matter air pollution and COVID-19 infection, severity, and mortality: a systematic review and meta-analysis. Sci. Total Environ. 880, 163272 (2023).
Google Scholar
Pompilio, A. & Di Bonaventura, G. Ambient air pollution and respiratory bacterial infections, a troubling association: epidemiology, underlying mechanisms, and future challenges. Crit. Rev. Microbiol. 46, 600–630 (2020).
Google Scholar
Herberth, G. et al. Maternal and cord blood miR-223 expression associates with prenatal tobacco smoke exposure and low regulatory T-cell numbers. J. Allergy Clin. Immunol. 133, 543–550e4 (2014).
Google Scholar
Haro-García, L. C. et al. Production of IL-10, TNF and IL-12 by Peripheral Blood mononuclear cells in Mexican workers exposed to a mixture of benzene–toluene–xylene. Arch. Med. Res. 43, 51–57 (2012).
Google Scholar
Bulog, A., Karaconji, I. B., Sutić, I. & Mićović, V. Immunomodulation of cell-mediated cytotoxicity after chronic exposure to vapors. Coll. Antropol. 35 (Suppl 2), 61–64 (2011).
Google Scholar
Bönisch, U. et al. Volatile organic compounds enhance allergic airway inflammation in an experimental mouse model. PloS One. 7, e39817 (2012).
Google Scholar
Kwon, J. W., Park, H. W., Kim, W. J., Kim, M. G. & Lee, S. J. Exposure to volatile organic compounds and airway inflammation. Environ. Health. 17, 65 (2018).
Google Scholar
Morrison, D., Rahman, I. & MacNee, W. Permeability, inflammation and oxidant status in airspace epithelium exposed to ozone. Respir Med. 100, 2227–2234 (2006).
Google Scholar
Liu, J. et al. Particulate matter disrupts airway epithelial barrier via oxidative stress to promote Pseudomonas aeruginosa infection. J. Thorac. Dis. 11, 2617–2627 (2019).
Google Scholar
Glencross, D. A., Ho, T. R., Camiña, N., Hawrylowicz, C. M. & Pfeffer, P. E. Air pollution and its effects on the immune system. Free Radic Biol. Med. 151, 56–68 (2020).
Google Scholar
Uzma, N., Kumar, B. S. & Hazari, M. A. H. Exposure to benzene induces oxidative stress, alters the immune response and expression of p53 in gasoline filling workers. Am. J. Ind. Med. 53, 1264–1270 (2010).
Google Scholar
Kirkeleit, J., Ulvestad, E., Riise, T., Bråtveit, M. & Moen, B. E. Acute suppression of serum IgM and IgA in Tank workers exposed to Benzene. Scand. J. Immunol. 64, 690–698 (2006).
Google Scholar
St Helen, G. et al. Differences in exposure to toxic and/or carcinogenic volatile organic compounds between Black and White cigarette smokers. J. Expo Sci. Environ. Epidemiol. 31, 211–223 (2021).
Google Scholar
Wahlang, B. et al. Associations between residential volatile organic compound exposures and liver injury markers: the role of biological sex and race. Environ. Res. 221, 115228 (2023).
Google Scholar
Wu, X. M. et al. Exposures to volatile organic compounds (VOCs) and associated health risks of socio-economically disadvantaged population in a ‘hot spot’ in Camden, New Jersey. Atmospheric Environ. Oxf. Engl. 1994. 57, 72–79 (2012).
Google Scholar
Schuyler, A. J. & Wenzel, S. E. Historical redlining impacts contemporary environmental and asthma-related outcomes in black adults. Am. J. Respir Crit. Care Med. 206, 824–837 (2022).
Google Scholar
He, T., Jin, L. & Li, X. On the triad of air PM pollution, pathogenic bioaerosols, and lower respiratory infection. Environ. Geochem. Health. 45, 1067–1077 (2023).
Google Scholar
Cohen, S. Social status and susceptibility to respiratory infections. Ann. N Y Acad. Sci. 896, 246–253 (1999).
Google Scholar
Gaffney, A. W., Himmelstein, D. U., Christiani, D. C. & Woolhandler, S. Socioeconomic Inequality in Respiratory Health in the US from 1959 to 2018. JAMA Intern. Med. 181, 968–976 (2021).
Google Scholar
Jbaily, A. et al. Air pollution exposure disparities across US population and income groups. Nature 601, 228–233 (2022).
Google Scholar
Michanowicz, D. R. et al. Home is where the Pipeline ends: characterization of volatile Organic compounds Present in Natural Gas at the point of the residential end user. Environ. Sci. Technol. 56, 10258–10268 (2022).
Google Scholar
Janasik, B., Jakubowski, M. & Jałowiecki, P. Excretion of unchanged volatile organic compounds (toluene, ethylbenzene, xylene and mesitylene) in urine as result of experimental human volunteer exposure. Int. Arch. Occup. Environ. Health. 81, 443–449 (2008).
Google Scholar
United States Environmental Protection Agency. Health Effects Notebook for Hazardous Air Pollutants.
link