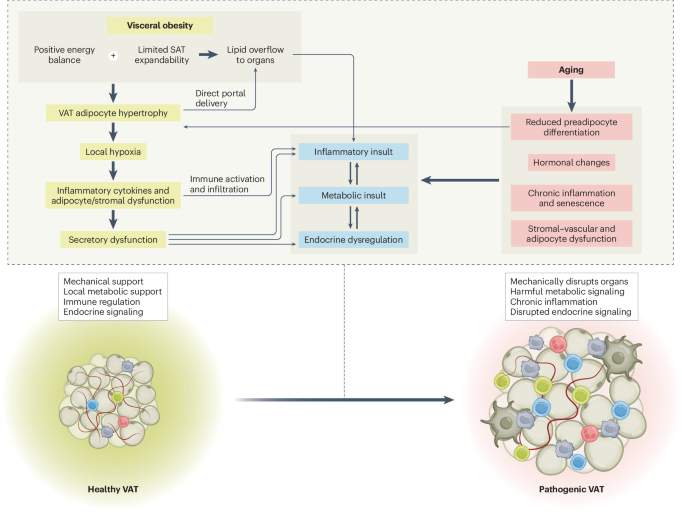
The correlation between different metabolic scores and the risk of cardiometabolic comorbidities in hypertensive patients
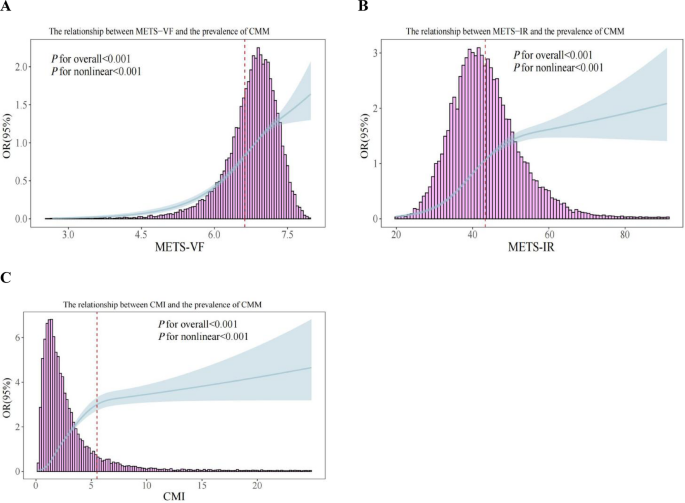
The findings of this study indicate that in the hypertensive population, higher levels of METS-IR, METS-VF, and CMI are associated with an increased risk of CMM. This relationship is particularly pronounced among male hypertensive patients. Our research not only validates the association between different metabolic scores and an elevated risk of CMM but also further reveals that METS-IR, METS-VF, and CMI have good predictive value for CMM. Notably, although previous studies have shown that cardiometabolic diseases are more common in the elderly population, our sensitivity analysis results indicate that even after excluding individuals over 50 years old, higher metabolic scores are still associated with an increased risk of CMM in hypertensive patients. The subgroup analysis revealed interactions between the three metabolic scores and gender, age, smoking, alcohol consumption, and BMI. Another significant finding was the nonlinear dose-response relationship between METS-VF, METS-IR, CMI, and the risk of CMM. These findings are consistent with previous research. The study by Cai21 demonstrated that the Cardiometabolic Index (CMI) was significantly associated with the risk of CMM in hypertensive patients. The study by Yang et al.22 also found that the Visceral Adiposity Metabolic Score (METS-VF) holds significant value in predicting future diabetes risk. Moreover, the study by Zhang et al.23 further substantiated the relationship between the metabolic score and the risk of CMM, highlighting the potential application value of the metabolic score in predicting CMM risk, indicating a close correlation between the metabolic score and CMM risk.
Cardiometabolic multimorbidity (CMM) is an increasingly concerning health issue24,25, particularly among the hypertensive population, as hypertension is the most common component of CMM26. Over 50% of hypertensive patients concurrently suffer from other cardiometabolic diseases such as diabetes and coronary heart disease27. A longitudinal cohort study involving millions of Chinese adults has shown that cardiometabolic multimorbidity significantly increases the risk of mortality28. Previous studies have indicated that hypertensive patients often exhibit higher metabolic scores29,30,31, and such metabolic abnormalities further elevate their risk of developing cardiometabolic multimorbidity32. The increased risk of comorbidity may stem from multiple mechanisms, including vascular dysfunction, oxidative stress, inflammatory responses, and lipid metabolism disorders33. In medical research and clinical practice, the presence of comorbidities has significant implications for patient diagnosis, treatment, and prognosis. Therefore, we included patients with hypertension as our study subjects to analyze the relationship between different metabolic scores and the risk of cardiometabolic comorbidities in hypertensive patients. The study results showed that the overall prevalence of CMM among hypertensive oil workers was 36.7%, higher than the 11.2% CMM prevalence reported in the study by Zheng Y et al.34 This discrepancy may be related to occupational specificity, regional environment, and differences in survey years. Shift work can disrupt circadian rhythms, affect dietary habits and sleep patterns, and consequently impact metabolic parameters35.Meanwhile, petroleum workers are often exposed to higher environmental pressures, which may lead to increased levels of psychological stress36, subsequently affecting metabolic status. Studies have shown37 that elevated stress levels are positively correlated with multiple components of metabolic syndrome, such as waist circumference, fasting blood glucose, and triglycerides. Additionally, the level of physical activity among petroleum workers may be influenced by the nature of their work. Although shift work does not significantly impact overall physical exercise, reduced physical activity during off-duty hours may affect metabolic health38. Moreover, the dietary habits in the Xinjiang region, characterized by high salt and fat intake and low consumption of fruits and vegetables, may further synergize with occupational factors to increase metabolic risks. In this study, the prevalence of CMM among women was 9.7%, lower than the 33.1% reported by Zhao Y et al.39 in their survey on the prevalence of cardiometabolic multimorbidity among Chinese women. The prevalence of CMM among men reached 34.3%, significantly higher than the 15.6% reported by Cheng et al.26 Trends in the Prevalence of Cardiometabolic Multimorbidity in the United States, 1999–2018. in their survey of the general male population in the United States. This discrepancy may be attributed to the predominance of male petroleum workers in this study (with males accounting for 86.69% of the study population), as men are more susceptible to accelerating cardiovascular pathologies by promoting insulin resistance and inflammatory responses, and thus typically exhibit higher visceral fat accumulation and cardiovascular risk40.
Furthermore, this study revealed significant multiplicative interactions between METS-VF, METS-IR, and CMI with alcohol consumption, and an antagonistic effect was observed between METS-VF and alcohol consumption. This phenomenon may be related to the complex regulatory effects of alcohol on lipid metabolism. The study by García-Villafranca et al.41 suggested that alcohol can inhibit AMPK-mediated lipolysis on one hand, and promote lipogenesis on the other. The research by Li Yuanyuan et al.42 indicated that alcohol has a dual regulatory role in lipid metabolism, promoting both triglyceride synthesis and fatty acid oxidation. This bidirectional regulatory effect may partially explain the antagonistic interaction observed between metabolic indicators and alcohol consumption in this study. METS-IR and CMI exhibited multiplicative interactions with gender and age, which may be related to Gender differences in hormonal regulation, fat distribution, and metabolic characteristics26. Males have higher levels of androgens, predisposing them to abdominal fat accumulation, whereas females benefit from the cardioprotective effects of estrogen before menopause. METS-IR showed an additive interaction with smoking. Smoking43, as a known risk factor for CMM, increases the risk of CMM through multiple pathways, including vascular endothelial damage, promotion of inflammatory responses, and disruption of lipid metabolism. As an indicator reflecting metabolism, the additive interaction between METS-IR and smoking suggests that elevated METS-IR levels further increase the risk of CMM in the smoking population.Similarly, the additive interaction between CMI and gender as well as BMI also suggests a similar risk accumulation effect. The age factor also exhibits a similar interaction, as the metabolic function of the human body gradually declines with age, and the relationship between metabolic scores and the risk of CMM may change with age. This finding is of significant importance for identifying high-risk populations and formulating targeted prevention strategies, indicating that these interaction factors should be comprehensively considered in clinical practice to more accurately assess an individual’s risk of CMM. CMI demonstrated the best performance in identifying CMM risk, with its higher AUC value and sensitivity (76.4%) being crucial for early screening and diagnosis of CMM, as early detection and intervention can effectively improve patient prognosis and reduce the incidence of complications. Although METS-IR and METS-VF showed better performance in AUC and specificity, they were slightly inferior to CMI in terms of sensitivity. Overall, the ROC curve analysis results of these indicators support our findings from the aforementioned interaction analysis: different metabolic scores play a significant role in identifying CMM risk, but their effects may be influenced by various subgroup factors such as gender, age, etc. Therefore, in clinical practice, it is necessary to combine multiple metabolic scoring indicators and clinical information for comprehensive evaluation to improve the accuracy of identifying CMM risk.
To the best of our knowledge, research on CMM is currently limited, although some have noted that dyslipidemia44, overweight, etc.45 are significantly associated with a gradually increasing risk of cardiometabolic multimorbidity. However, there is no research on the correlation between metabolic scores in hypertensive patients and the risk of CMM. Nevertheless, hyperlipidemia, hyperglycemia, and obesity are important and modifiable risk factors for hypertensive patients. By integrating these metabolic indicators to more accurately assess the risk of CMM, it can help better evaluate the risk of its onset and formulate new preventive strategies.
This study also has certain limitations. Firstly, it is a cross-sectional study that can only reflect the disease and exposure status of individuals at the time of the survey, and cannot determine causal relationships. Secondly, the sample of this study is from a single-center sample of occupational populations in Xinjiang, and its extrapolation has certain limitations. Thirdly, CMM was measured through self-reported chronic diseases, and thus may be underestimated or overestimated in this study. Future large-sample longitudinal epidemiological studies are still needed for different regions and populations. Therefore, prospective cohort studies will be conducted in the future to test etiological hypotheses, further verify the association between metabolic scores and CMM in hypertensive patients, and provide a scientific basis for early identification of high-risk CMM populations and the formulation of corresponding effective personalized prevention and intervention strategies.
link